
Periodontal Disease
Chronic periodontal disease is a lasting bacterial infection which has harmful effects on the bones that support one’s teeth as well as the gums and tissues surrounding one’s teeth. It has been determined by a variety of studies that some 75 percent of adult tooth loss is due to the existence of periodontal disease. Periodontal disease does not discriminate; it can have an effect on one or all of an individual’s teeth, and it can affect individuals of all ages, genders, and races. The onset of periodontal disease and issues with the gums is instigated by plaque and the bacteria in plaque in most cases. Plaque is a colorless film that forms on the teeth continuously; the substance is sticky and clings to one’s teeth, which later causes the gums to be severely irritated and infected.
What is periodontal disease? It is a disease occurring in the mouth of an individual that, over time, can produce a loss of teeth, as well as a variety of other major health issues. Periodontal disease is something that needs to be treated by a trained periodontist as soon as possible to secure the longevity of one’s oral health.
Periodontal (gum) diseases is a chronic bacterial infection that affects the gums and bone supporting the teeth. Periodontal disease includes gingivitis and periodontitis, and if left untreated, it can lead to tooth loss. The word periodontal means “around the tooth.” Periodontal disease can affect one tooth or many teeth. It begins when the bacteria in plaque (the sticky, colorless film that constantly forms on your teeth) causes the gums to become inflamed. The harmful effects of gum disease include potential tooth loss, and individuals can actually have periodontal disease and not even be aware that they have it until the condition worsens.
Please click a link below to obtain more information about periodontal disease.
Gingivitis
Gingivitis is the mildest form of periodontal disease. It causes the gums to become red, swollen, and bleed easily. There is usually little or no discomfort at this stage. Gingivitis is often caused by inadequate oral hygiene. Gingivitis is reversible with professional treatment and good oral home care.
Periodontitis
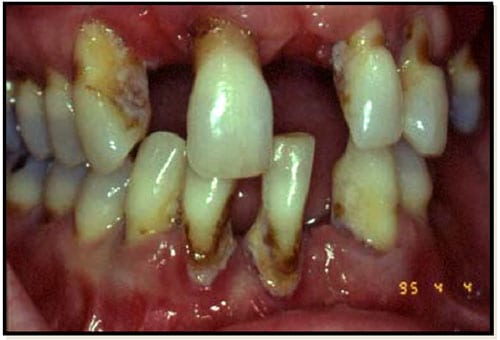
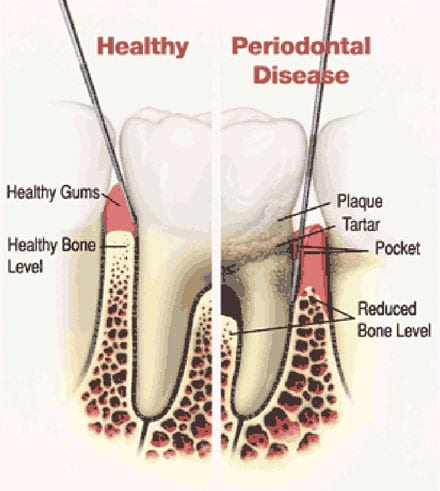
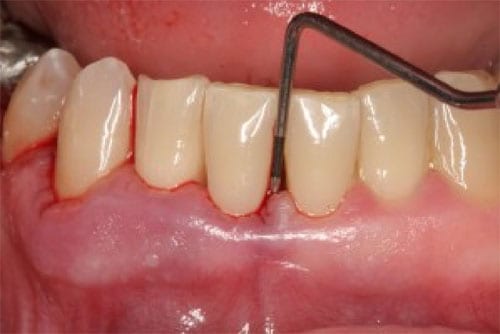
Aggressive periodontitis occurs in patients who are otherwise clinically healthy. Common features include rapid attachment loss and bone destruction and familial aggregation.
Chronic periodontitis results in inflammation within the supporting tissues of the teeth, progressive attachment and bone loss. This is the most frequently occurring form of periodontitis and is characterized by pocket formation and/or recession of the gingiva. It is prevalent in adults, but can occur at any age. Progression of attachment loss usually occurs slowly, but periods of rapid progression can occur.
Necrotizing periodontal disease is an infection characterized by necrosis of gingival tissues, periodontal ligament and alveolar bone. These lesions are most commonly observed in individuals with systemic conditions such as HIV infection, malnutrition and immunosuppression.
Symptoms of Periodontal Disease
What are the symptoms of periodontal disease? In its early stages, one can have periodontal disease without being aware of it. This is why it is very necessary for people to get regular dental checkups and evaluations so that a trained professional in the field of dentistry can identify if the individual has periodontal disease. As periodontal disease progresses and the periodontal infection gets worse, an individual will be able to recognize that he or she has periodontal disease by the following signs and symptoms:
- The chronic presence of bad breath and gingivitis
- Red, irritated, and swollen gums
- Gums bleeding after brushing (a toothbrush may appear reddish or pink after brushing)
- Sore and achy gums
- Itchy gums
- Gum recession (individual’s teeth will have a longer appearance than usual)
- Pain and irritation upon flossing
- Increasing gaps forming between the teeth
- Tooth loosening and tooth loss
- Improperly fitting dentures or appliances
- Minor to significant changes in one’s jaw-line or bite
- Difficulty eating and chewing
- Tooth sensitivity
Any of the above symptoms, either singularly or combined, is an indication that an individual should seek out a professional like a certified periodontist. The signs listed above are indicative of periodontal infection which requires treatment in order to restore one’s oral health. One should contact a general dentist or certified periodontist as soon as possible to schedule an evaluation and to develop a plan of treatment.
An individual with periodontal disease can look perfectly normal and still have periodontal infection forming in the deep pockets around the teeth. Only a qualified dentist or periodontist can advise an individual whether or not one actually has periodontal disease or the early signs of such a disease. That is why regular checkups are so important.
Access the American Academy of Periodontology’s self-assessment tool to see if you might have issues with periodontal disease now.
Causes of Periodontal Disease
The Primary Cause is Plaque and Plaque Build Up
So what causes periodontal disease or gum disease? There are several things that can cause one to get periodontal disease; one of the primary causes however is plaque and the bacteria that lives and thrives in plaque. Plaque is constantly forming in one’s mouth and sticking to one’s teeth. Appropriate removal through brushing and flossing can help to reduce the amount of plaque in one’s mouth, but sometimes even these precautionary measures are not enough. Regular dental checkups and cleanings can also help reduce the amount of plaque buildup on one’s teeth. Nevertheless, sometimes as people age, issues with periodontal disease arise. This is where the services offered by a professional periodontist can work for you, helping you keep your smile, your mouth, and your entire body healthier.
Secondary Causes
There are factors that can contribute to the onset of periodontal disease. Below are some of the secondary factors that play a role in the appearance of gum disease.
Tobacco Use, Smoking, and Periodontal Disease
It is well known that smoking is bad for you, but did you know that it actually plays a role in the onset of periodontal disease? In addition to causing diseases such as cancer and heart disease, smoking is responsible for a variety of health issues including periodontal disease. Studies have revealed that when an individual smokes, the likelihood that the individual will get periodontal disease increases tremendously, and once periodontal disease develops, smoking can hasten the progression of gum disease as well.
Genetics and Periodontal Disease
Studies are revealing the role that genetics have in the onset of gum disease. Recently noted is the fact that just under one-third of the population, as much as 30% of all people will get gum disease because they are genetically predisposed to get it. Even with good oral hygiene and regular checkups, it is possible for people to get gum disease. For those individuals that are genetically predisposed to periodontal disease, early intervention is needed for successful treatment. The appropriate periodontal care will ensure that the individual can maintain maximum oral health as well as keep their natural teeth for the rest of their natural lives.
Pregnancy, Puberty, Menopause, and Gum Disease
Women face unique health needs and this includes unique dental needs as well. While a woman can take care of herself with appropriate diet and exercise, a good oral hygiene regimen, and regular care from a physician as well as a professional dentist, it is still very possible to develop gum disease. In fact, there are certain stages in a woman’s life where the potential for developing gum disease increase: such stages include puberty, pregnancy, and menopause.
Hormonal changes have a significant role in the types of health needs that a woman has; when hormonal changes affect a woman’s body it can have an overall effect on a woman’s bodily tissues and such tissues include the gums. In fact, in some instances, hormonal changes can affect a woman’s gums and make them ultrasensitive, tender, and more prone to develop gum disease.
Gum disease has a terrible effect on women and their bodies. Researchers are now discovering just how bad gum disease can be; there are studies currently revealing that women with periodontal disease are seven times more apt to have babies delivered preterm and/or with low birth weights. Thus, women must address their unique bodily needs in terms of health care, and seek out the professional care of a qualified dentist and/or the best periodontist.
Periodontal Disease and Stress
Stress is responsible for the onset of many harmful conditions, including periodontal disease. Stress not only causes high blood pressure, cardiac health issues, and is also believed to be linked with certain types of cancers, but stress also increases the likelihood that one will develop gum disease. Stress has a direct affect on one’s immune system functioning which, in turn, weakens one’s ability to fend off infection: including periodontal infection and periodontal disease.
Medications and Gum Disease Onset
Believe it or not, even certain medications may increase the likelihood that an individual will get periodontal disease. For instance, a heavy reliance on antibiotics can weaken one’s immune system and one’s ability to fight infection. Oral contraceptives, the use of heart medications, and the use of anti-depressants may also play a role in the onset of gum disease. A professional Periodontist can determine if your medicines are placing you at a higher risk for getting gum disease and can help you implement changes to prevent gum disease in the future.
Teeth Grinding and Teeth Clenching
When you grind or clench your teeth on a regular basis, you are doing more than merely damaging your teeth over time. You could be increasing the chances of getting gum disease. Excessive force on your teeth also affects the surrounding tissues of your teeth as well and can increase the rate in which such tissues are destroyed. Teeth grinding and teeth clenching are treatable conditions, and as such, should be remedied so that you lessen your chances for getting gum disease in the future.
Diabetes and Periodontal Disease
A disease like Diabetes has a number of different effects on the individual. First, sugar levels are altered in the individual that has diabetes. The onset of Diabetes occurs when there is not enough insulin in one’s body or the body does not utilize the insulin it has correctly. Either way, Diabetes is a disease that opens up an individual to a whole host of other issues, including increased infections. The American Diabetes Association suggests that more than 16 million U.S. citizens actually have the disease, but only a mere 8 million are aware that they have it. As a Diabetic, an individual can get gum disease with relative ease, and gum disease in a Diabetic can prove worse than gum disease in an individual that does not have Diabetes; thus, care by the best periodontist one can find is necessary.
Medical Consequences
Periodontal disease is a significant problem in the United States. Many people suffer from gum disease and do not even realize it. A dreadful infection, periodontal disease releases bacteria into an individual’s bloodstream and therefore causes a whole host of other health complications. Gum disease is not solely a dental issue; it has a myriad of effects on one’s overall health and general well being.
Periodontal disease is no longer thought of as just a dental problem. Research is finding many correlations between periodontal infection and serious medical problems. Below, some of the complications associated with gum disease are indicated and examined.
Cardiac Issues and Strokes
Periodontal disease can increase the chances of having a heart attack. Scientists have discovered that if an individual has gum disease, he or she is 2.7 times more likely to suffer from a heart attack. One also has an increased chance for having a stroke. Periodontal disease can increase an individual’s risk of having a stroke three times.
Women’s Health and Gum Disease
Individuals suffering from diabetes are three to four times more likely of developing periodontal disease, and patients with untreated chronic periodontal infections can cause diabetes to be more difficult to control. Diabetic patients have more severe levels of bone loss around their teeth, often experience acute episodes of more aggressive disease activity, and ultimately leading to tooth loss.en with periodontal disease are 7 times more likely of having a preterm birth, or having babies with a low birth weight. A woman should ensure that her teeth and gums are healthy before becoming pregnant to ensure a healthy baby and delivery.
Diabetes
Individuals suffering from diabetes are three to four times more likely of developing periodontal disease, and patients with untreated chronic periodontal infections can cause diabetes to be more difficult to control. Diabetic patients have more severe levels of bone loss around their teeth, often experience acute episodes of more aggressive disease activity, and ultimately leading to tooth loss.
Periodontal Disease and Respiratory Disease
With the onset of periodontal disease, an individual is more likely to become ill with other diseases. Periodontal disease can cause respiratory issues when the periodontal infection is inhaled via the mouth. Complications with diseases like bronchitis, emphysema, and pneumonia can result in an individual suffering from gum disease.
Periodontal Bacteria is Transmissible?
There is evidence that bacteria that causes periodontal disease is transmissible. Scientists utilizing advanced DNA testing and technology have demonstrated that if an individual has gum disease, the bacteria associated with the disease can be passed on to one’s spouse and/or children.








